New Stem Cell Research Shows Promising Results for Muscular Dystrophy
The term muscular dystrophy (MD) refers to a group of disorders in which a genetic abnormality causes muscles responsible for controlling movement to become weak, and muscle mass to be lost. These inherited disorders usually affect voluntary (skeletal) muscles, although weakness can also extend to the muscles that control respiration and swallowing.
Given that the genetic mutations triggering MD interfere with the normal production of certain critical proteins, the body is not able to reverse muscle weakening or loss of mass, so even when the disease progresses slowly, it eventually affects one’s ability to walk in a more or less conducive manner.
Who is affected by muscular dystrophy?
In most cases MD appears in infancy, but it’s not uncommon for symptoms to start manifesting in teens or adults.
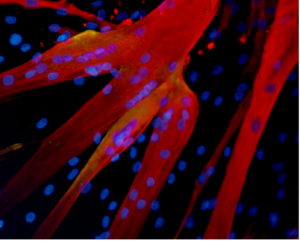
Muscle fibers formed in the lab by human mesoangioblasts (image: eurostemcell).
There are different kinds of muscular dystrophy, the most common and severe form being Duchenne muscular dystrophy (DMD) Caused by a genetic flaw or defect, Duchenne MD is more common in males than females [1} and affects about 1 in every 3,500 boys worldwide.
The onset of Duchenne muscular dystrophy occurs between the ages of 2 and 6, and evolves slowly. Muscles becoming weaker year after year, and the spine and limbs becoming progressively deformed. In most cases, children affected by this form of the disease become wheelchair dependent by the age of 12.
People suffering from Duchenne MD often die in their 20s, and those who survive usually experience some degree of cognitive impairment. The shortening of tendons and muscles limits the mobility of sufferers even more, and breathing and heart problems can occur.
Treatments for Duchenne muscular dystrophy
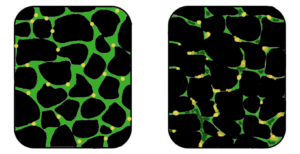
Muscular dystrophy is a genetic disorder where the muscle tissue wastes away and loses function. In the affected muscle (left), the tissue has become disorganized and the concentration of dystrophin (green), an important protein in normal muscle functioning, is greatly reduced. (Image: Wikipedia)
Physiotherapy is commonly used for slowing down the loss of muscle mass and for maintaining flexibility or reducing muscle stiffness. Steroids are also used to slow down muscle wasting, but the severe side effects of steroids often cause more harm than good, such as bone weakening or cardiovascular problems.
In a healthy organism, damaged muscles repair themselves thanks to a series of cells that include muscle stem cells, called satellite cells. In Duchene muscular dystrophy, the muscles lack dystrophin, the protein needed for maintaining the integrity of muscle fibers. Without this protein, the burden placed on the body’s naturally occurring muscle stem cells is too intense, rendering the cells unable to repair damaged muscle tissue or to generate new muscle mass to replace wasted mass [6].
For this reason, scar tissue and fat cells take the place of damaged muscle tissue, contributing to muscle weakening and, over time, cause muscles to lose their functional ability. Would it be possible for the damaged muscle fibers to regain their regenerative ability with help from transplanted stem cells?
Research suggests stem cells could be a potential solution for muscle wasting
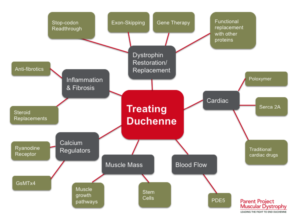
(Click on image to enlarge) Considerable efforts are underway to develop drugs and biologics (cell and gene therapy) to address the primary problem in Duchenne—the absence of dystrophin. Restoring dystrophin or replacing dystrophin with replacement protein are considered foundational therapies.
In 2006, researchers managed to restore mobility in two afflicted dogs using stem cells isolated from muscle blood vessels [4], and in 2007 scientists managed to treat Duchenne MD in research mice using a combination of genetic correction and stem cells [3]. The latter study showed that it is possible to correct the genetic error in the cells that no longer produce dystrophin protein, and inject corrected cells stimulating the regeneration of muscles.
Researchers at the Harvard Stem Cell Institute obtained similar results, demonstrating that transplanted muscle stem cells can improve function in mice with MD, while replenishing the stem cell population in muscle fibers [5].
Although it’s still too early to say whether stem cells can cure DMD in humans, it’s clear that there are some promising stem-cell-based approaches for Duchenne MD. One solution is to replace the defective stem cells with healthy stem cells, as these may be able to generate working muscle fibers to replace damaged muscle fibers .
A second solution would be to reduce the inflammation that speeds up the loss and weakening of muscles using certain types of stem cells [2]. Combined treatments, such as mixing stem cell therapies with gene therapies are also being tested and may prove successful in the near future.
References:
- http://www.mayoclinic.org/diseases-conditions/muscular-dystrophy/basics/definition/con-20021240
- http://www.eurostemcell.org/factsheet/muscular-dystrophy-how-could-stem-cells-help
- https://www.mda.org/disease/duchenne-muscular-dystrophy/research
- http://quest.mda.org/article/scientists-bullish-stem-cells-muscle-repair
- http://hsci.harvard.edu/stem-cells-used-treat-muscular-dystrophy-mice
- https://med.stanford.edu/news/all-news/2014/12/stem-cells-faulty-in-duchenne-muscular-dystrophy.html
- Published in Corporate News / Blog
Stem cells may be used for healing damaged lungs
Healing damaged lungs with stem cells.
A New study published by scientists from the Weizmann Institute of Science suggests that stem cells may be used for repairing damaged lung tissue. This discovery gives new hope for treating conditions like bronchitis, asthma, cystic fibrosis or emphysema, which affect more than 35 million Americans and are the second leading cause of death worldwide.
[su_spacer]
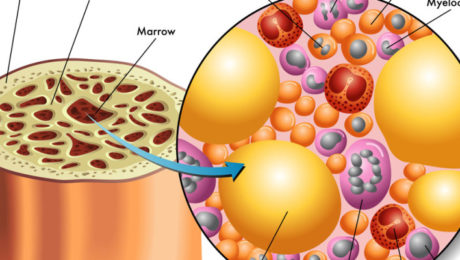
Bone Marrow stem cells able to generate new lung tissue
The treatment method proposed by scientists at the Weizmann Institute is based on the similarities between stem cells that reside in the lungs and those in bone marrow. Bone marrow stem cells, when transplanted to a patient, manage to find their way through the blood and to navigate to the designated area where they differentiate.
 Acknowledging the similarities between lung and bone marrow stem cells, Professor Yair Reisner of the Immunology Department of the Weizmann Institute tested the ability of lung stem cells to travel to a specific region after transplantation in mice [1]. Before introducing the bone marrow stem cells into mouse models with lung damage, the group of scientists cleared the lungs’ stem cell compartments to clear a path for the transplanted cells.
Acknowledging the similarities between lung and bone marrow stem cells, Professor Yair Reisner of the Immunology Department of the Weizmann Institute tested the ability of lung stem cells to travel to a specific region after transplantation in mice [1]. Before introducing the bone marrow stem cells into mouse models with lung damage, the group of scientists cleared the lungs’ stem cell compartments to clear a path for the transplanted cells.
The injected stem cells managed to reach the empty lung compartments and settle in the lungs, where they differentiated into normal lung tissue,six weeks after transplantation. Results showed that new lung cells continued to be created from the transplanted stem cells 16 weeks after the implantation, ultimately healing the damaged lungs and improving their breathing ability.
The Weizman scientists intend to continue their research by exploring this option further, and possibly create a bank of lung stem cells that can provide cells ready to be transplanted to patients with severe respiratory diseases.
Lung-specific induced pluripotent stem cells (iPSCs)— potential alternative to bone marrow stem cells
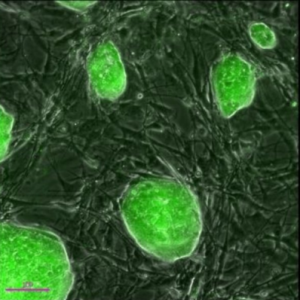
Mouse iPSCs generated using the microRNA method pioneered by the Morrisey Lab. The green fluorescence reveals expression of the Oct4 gene, (Image: Science Daily).
Darrell Kotton, the study’s lead author, highlighted the fact that iPSCs are easier to cultivate in lab conditions than bone marrow stem cells, and are genetically identical to the patient’s cells, so the risk of rejection in such transplants is eliminated. The lung-specific iPSCs obtained by manipulating adult stem cells into a primitive stem cell state could solve some of the hurdles impacting other kinds of stem cell research.
In this study, scientists used skin stem cells manipulated into primitive pluripotent stem cells, with results showing that the iPSCs have the ability to multiply and differentiate into endoderm tissue–the natural precursor of lung cells [2].
References:
- Chava Rosen, Elias Shezen, Anna Aronovich, Yael Zlotnikov Klionsky et al. – Preconditioning allows engraftment of mouse and human embryonic lung cells, enabling lung repair in mice, Nature Medicine, 2015, http://www.nature.com/nm/journal/vaop/ncurrent/full/nm.3889.html
- Aba Somers, Jyh-Chang Jean, Cesar A. Sommer, Amel Omari et al. – Generation of transgene-free lung disease-specific human induced pluripotent stem cells using a single excisable lentiviral stem cell cassette, Stem Cells, 2010, 28 (10):1728, http://onlinelibrary.wiley.com/doi/10.1002/stem.495/full
- Published in Corporate News / Blog
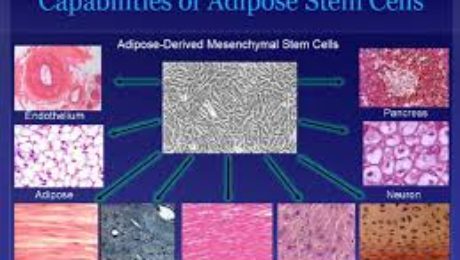
Adult tissues that serve as sources for stem cells
Where do adult stem cells come from?
Adult stem cells receive much interest in the scientific community thanks to their ability to self-renew and generate numerous types of cells and tissues. There are two categories of stem cells: embryonic and adult.
Unlike embryonic stem cells, which have the ability to differentiate into more than one cell type, most adult stem cells are capable of forming only the types of tissue from which they originated. However, due to the controversy surrounding embryonic stem cell use, more and more researchers have turned their attention to the study of adult stem cells.
As a result, we now know of several adult tissues that serve as sources for stem cells. This is great news for people who suffer from degenerative conditions like osteoarthritis, muscular dystrophy and even Alzheimer’s disease.
The list of adult tissues known to contain stem cells keeps growing, and it includes bone marrow, brain tissue, peripheral blood and blood vessel tissue, skeletal muscle tissue, and liver and pancreas tissue.
Adult stem cells can be obtained from multiple tissues
Neural brain cells (NSCs) are multipotent cells that generate the central nervous system. They undergo asymmetric cell division, resulting in one non-specialized (blank) cell and one specialized cell. Japanese researchers have been able to use NSCs to replace dying neurons in lab mice [1]. Currently there are numerous ongoing investigations into the response of NSCs in multiple sclerosis (MS) and Parkinson’s disease patients. The results may have future applications in the treatment of additional neurological conditions.
Hematopoietic stem cells (HSCs) are stem cells harvested from blood or bone marrow. They can differentiate into variety of specialized cells, such as white blood cells, which fight infection, and red blood cells, which carry hydrogen and platelets, and are responsible for blood clotting.
The downside of HSC stem cells is that their ratio in bone marrow is very low—1 in every 10,000-15,000 cells, which slows down the harvesting process considerably. Bone marrow also hosts skeletal stem cells (STCs), which give rise to osteoblasts (bone cells), cartilage and hematopoietic stroma.
An interesting niche of stem cells is found in the surface lining of the small and large intestines (ISCs). These stem cells divide continuously throughout life and are believed to be the source of most forms of cancer of the small intestine and colon. The longevity and renewal rates of ISCs becomes problematic in colorectal cancer, because they promote regeneration of the tumor after therapy.
In healthy adults, the liver is responsible for maintaining the balance between cell gain and cell loss. The liver’s impressive regenerative functions are attributed to hepatocytes, which are believed to be the adult stem cells of the liver. When the liver tears apart from virus infections, inflammation or is sectioned through hepatectomy, hepatocytes activate a stem cell-like behavior, giving rise to new tissue, replacing the lost liver cells.
Another important discovery has been made by Dr. Lola Reid of the University of North Carolina, an accredited expert in the research of liver development [2]. As it turns out, the biliary tree, a network of vessels that connect the liver and pancreas to the intestine, generates a special type of adult stem cells, their major characteristic being pancreatic precursor cells, meaning they are destined to differentiate as pancreatic cells.
In a series of lab tests, these biliary cells have been manipulated to become islets, structures responsible for the production of insulin and c-peptide, a key component in the natural production of insulin. As a result, the blood sugar control in has been found to increased dramatically in lab mice. Dr. Reid hopes that her team’s efforts will speed up the process of finding a cure for diabetes.
Over the past few decades, scientific research has provided us with great insight on adult stem cells and their applications in regenerative medicine.
Unlike embryonic stem cells, adult stem cells can be isolated from a variety of adult tissue, including the brain, bone marrow, peripheral blood and even tumor-derived tissue cells, allowing scientists to avoid the ethical dilemma of using embryonic stem cells entirely. The risk of rejection with adult stem cells is considerably lower (the donor is usually the patient himself), and the differentiation rates are higher, providing much hope for future research to find cures for degenerative conditions in humans.
REFERENCES:
[1] MacKlis, Jeffrey D.; Magavi, Sanjay S.; Leavitt, Blair R. (2000). “Induction of neurogenesis in the neocortex of adult mice”. Nature 405 (6789): 951–5[2] Biliary Tree Stem Cells, Precursors to Pancreatic Committed Progenitors: Evidence for Possible Life-long Pancreatic Organogenesis – http://www.diabetesresearch.org/file/research-publications/2013-Stem-Cells_Biliary-Tree-Stem-Cells-to-Islets.pdf
- Published in Corporate News / Blog
We may soon be able to heal autoimmune disorders with Stem Cells
Autoimmune disorders are conditions in which the sufferer’s body produces substances that attack the healthy cells of the organism, as it doesn’t distinguish between the healthy tissues and antigens. There are more than 80 types of autoimmune conditions known today, among which diabetes type 1, systemic lupus erythematosus, rheumatoid arthritis, celiac disease, myasthenia gravis and multiple sclerosis.
The exact cause of these ailments is unknown, but scientists believe that viruses, bacteria or certain drugs may trigger some internal changes that confuse the organism and cause the immune system to react by destroying the healthy tissues. Besides the damage caused to healthy cells, autoimmune conditions also lead to changes in organ function and may cause the abnormal growth of organs.
These disorders may affect several tissues or organs, but the most common areas that are destroyed by the immune system include the red blood cells, skin, connective tissues, blood vessels, endocrine glands (mostly the pancreas and thyroid), joints and muscles.
Currently, the standard treatment for autoimmune conditions is represented by immune suppressive agents, but these medications only induce temporary improvements, and don’t cure the disorders completely. For this reason, scientists have started to investigate the potential use of stem cells in autoimmune disorders.
In animal studies, stem cell therapy with mesenchymal stem cells has been shown to induce healing activity in various autoimmune disorders, and to prevent the destruction of healthy tissues by the immune system. But what does research say about treating autoimmune disorders in humans? Are stem cells effective in this case as well?
THE USE OF STEM CELLS IN AUTOIMMUNE DISORDERS IN HUMANS
Mesenchymal stromal stem cells have been found to exert immunological functions under inflammatory conditions, a study published by researchers at the Department of Internal Medicine, Erasmus MC, Rotterdam in Arthritis Research and Therapy showing that MSCs play an important role in maintaining immune homeostasis [1].
According to researchers, MSCs do not have immune cell effector functions and are not “true” immune cells, but can play a role in the initiation of immune responses. Unlike immune T- and B-cells, mesenchymal stem cells do not poses receptors for recognizing the antigens, but they do express pattern recognition receptors, which enable the stem cells to recognize microbes.
In conclusion, the mentioned study showed that although MSCs do not fit the exact definition of immune cells, they do influence the body’s immune response and can act as regulators or coordinators of the immune system [1].
In another paper published in the Nature journal, scientists at the Massachusetts General Hospital, Harvard Medical School have showed that hematopoietic stem cells may be used in treating severe autoimmune diseases, like rheumatoid arthritis or multiple sclerosis [2].
The stem cell therapy investigated by the US researchers involved the transplantation of HSC following an immunosuppressive treatment like chemotherapy or radiotherapy. This treatment was found to be effective in curing autoimmune diseases in animal models, and most patients who received allo-HCT achieved remission of the disorder, although there were also exceptions.
Researchers at the Stem Cell Technology Research Center, Tehran have investigated the use of stem cell therapy in multiple sclerosis patients. Their review paper, published in the International Journal of Hematology-Oncology and Stem Cell Research, showed the following: neural stem cells derived from the adult central nervous system may have neuroprotective and immunomodulatory effects, so they may be a solution for treating MS [3].
Mesenchymal stem cells derived from bone marrow also have a potential for migration into the inflamed tissues of the central nervous system and are able to differentiate into neuronal cells. In mice, MSCs helped in improving the neurological function of animals with experimental autoimmune encephalomyelitis (EAE). The application of stem cells in humans with multiple sclerosis was also investigated by scientists at the American University of Beirut Medical Center, Lebanon, who showed that bone marrow mesenchymal stem cells may lead to clinical improvements in patients with advanced multiple sclerosis [4].
Another autoimmune condition in which stem cells may be useful is rheumatoid arthritis, studies showing that human amnion mesenchymal cells isolated from the placenta may be feasible for treating collagen-induced arthritis in rats [5]. These cells have immunosuppressive functions and can ameliorate the severity of arthritis, so they may be a promising therapy for RA sufferers.
Despite these positive results, there are still a lot of challenges to overcome when it comes to treating autoimmune disorders with stem cells, so scientists need to establish precise protocols for all these conditions that could be treated through stem cells therapy.
References:
[1] http://www.arthritis-research.com/content/17/1/88
[2] http://www.nature.com/nature/journal/v435/n7042/full/nature03728.html
[3] http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3913133/
[4] http://www.ncbi.nlm.nih.gov/pubmed/20728948
[5] http://www.ncbi.nlm.nih.gov/pubmed/25962385
- Published in Corporate News / Blog
STANFORD RESEARCHERS ISOLATE SKELETAL STEM CELLS THAT GIVE RISE TO BONES AND CARTILAGE
Cartilage and bone deterioration are a common consequence of aging, but poor diet, sedentary lifestyle, excess weight or injury can also result in damaged tissue. Unlike bone tissue, mature cartilage is avascular and doesn’t heal well after injury. Replacement or augmentation surgery is one way to fix a torn joint, but the costs are high and there are also several risks involved in the procedure, such as transplant rejection and infection [1].
In January 2015, scientists at the Stanford University School of Medicine published a paper regarding their latest findings in tissue engineering. With the use of skeletal stem cells (myoblasts), they have been able to give rise to bone and cartilage in mice. In addition, they mapped out the chemical signals which can create skeletal muscle stem cells, directing their development into specialized types of cells [2].
To better understand the medical significance of these findings, we are going to take a closer look at stem cells and their role in bone and cartilage regeneration.
HOW SKELETAL STEM CELLS ARE OBTAINED
Stem cells (or blank cells) are undifferentiated cells that can divide or differentiate into specialized cells, replacing dying cells or damaged tissues. There are two broad types of stem cells: embryonic stem cells (ESCs) and adult stem cells (somatic stem cells).
ESCs are harvested from embryos 4-5 days post-fertilization, at each time they consist of 50-150 cells. Embryonic stem cells are pluripotent and can repair damaged tissue or stimulate the regeneration of diseased cells. However, due to ethical controversy, the study of ESCs is a slow process.
In humans, bone marrow, peripheral blood and adipose tissue are rich sources of adult stem cells, but these can be also harvested from some brain areas, skin, liver and even teeth. Until recent years, it was thought that adult stem cells differentiate only as the type of tissue they originate from. Emerging studies suggest that just like ESCs, these cells can specialize in unrelated cell types, as well.
The study conducted at the Stanford University School of Medicine supports these claims. The research focused on groups of cells with a fast division rate, located at the ends of mouse bones. Human skeletal muscle-derived cells were transplanted into host mice.
Prior to the procedure, the targeted host tissues were modulated by irradiation and cryoinjury, to allow the observation of the transplanted cells in mice. After four weeks of observation it was discovered that these isolated collections of cells were able to reconstruct all parts of the mouse bone.
Through further investigation, scientists were able to map the developmental tree of skeletal stem cells, which provided great insight on how to give rise to more specific types of cells. Irving Weissman, MD professor of pathology and of developmental biology, who directs the Stanford Institute for Stem Cell Biology and Regenerative Medicine, hopes that once these findings are translated into humans, the odds of rescuing cartilage and bone from wear and aging will increase significantly [3].
DIFFERENTIATION OF SKELETAL STEM CELLS AND THERAPEUTIC APPLICATIONS
Skeletal muscle is a dynamic tissue, capable of a regenerative response within a couple of weeks. This ability is primarily due to its satellite cells populations, a type of cells that are located peripheral to the myofiber.
When injury or disruption occurs, these satellite cells become activated and either fuse together to replace the damaged myofiber or multiply at an increased rate, supporting additional rounds of regeneration. In addition, skeletal stem cells can also give rise to blood derivatives, vascular components, osteoblasts (bone formation cells), adipocytes (fat cells) and cartilage [4].
The use of skeletal stem cells for therapeutic purposes brings hope to patients who suffer from muscular conditions, including muscular dystrophy. Joint pain, dislocations and arthritis are also on the list of potential stem cell therapy. Rheumatoid arthritis, Osteoarthritis and even Multiple Sclerosis patients could also benefit from these findings in the not-too-distant future.
The main challenge of using myoblasts for cell therapy remains, for now, harvesting and culturing them up to the numbers required.
References
[1] David King – Development and remodeling of skeletal tissue, School of Medicine, Southern Illinois University, 2009 http://www.siumed.edu/~dking2/ssb/skeleton.htm#development
[2] Christopher Vaughan – Researchers isolate stem cell that gives rise to bones, cartilage in mice, Stanford Institute for Stem Cell Biology and Regenerative Medicine, 2015 https://med.stanford.edu/news/all-news/2015/01/researchers-isolate-stem-cell-that-gives-rise-to-bones-cartilage.html
[3] http://www.stemcellclinic.net/tag/stanford
[4] http://genesdev.cshlp.org/content/20/13/1692.long
- Published in Corporate News / Blog
PROTEINS PRODUCED BY STEM CELLS, USED IN BONE REGENERATION
The loss of bone mass and the weakening of the bones are natural consequences of aging, but this process starts around the age of 30, so it’s not only the elderly that are at risk for falls and fractures due to bone resorption.
Some of the factors that cause the decrease in bone mass density can be controlled, but others are out of one’s control. Smoking for example can be avoided, and one can practice strength exercises to keep their bones strong, but an inadequate intake of calcium, the use of asthma medications, as well as the changes in hormone levels that occur in older adults can speed up the weakening of bones.
Also, this process is accelerated by an inadequate intake of vitamin D, the lack of exposure to gravity and hypoparathyroidism, all these factors favoring the resorption of bone. When the tissue is broken down faster than it can be renewed, the density of bones starts to decrease and they become more porous, fragile and prone to fractures.
Although there are a series of conventional treatments that can help in improving bone density in osteoporotic patients, people who suffer multiple fractures, major bone trauma or individuals injured during natural disasters may require a different approach. In such cases, the use of stem cells could speed up bone repair and eliminate the risk of tumor formation.
STEM CELLS FROM BONES AND SKIN, USED FOR BONE RECONSTRUCTION
Scientists from the Gladstone Institutes have discovered a way to stimulate bone reconstruction using proteins produced by stem cells. Instead of grinding up bones from cadavers in order to extract the proteins and growth factors needed for stimulating the growth of new tissue, the researchers have extracted bone-forming proteins from stem cells.
After they treated the proteins in the lab, they injected the substances into muscle tissue of mice, in order to facilitate bone growth. The injected proteins were effective in creating new bone tissue, so there is hope that this method may be a good solution for humans as well. Unlike current treatments, the use of stem cells is safer as it doesn’t involve the transplant of cells or tissues from cadavers or other donors, so the risk for these cells to be rejected is much lower and the risk for tumor formation is very low also.
The study published in Scientific Reports concluded that proteins extracted from stem cells could be a consistent and reproducible source material for tissue regeneration [1]. This isn’t the first study to support the use of stem cells for orthopedic purposes. In 2001, another paper published by Dr. Ranieri Cancedda in the New England Journal of Medicine described the use of autologous bone marrow cells in the repairing of large bone defects.
The research showed that the osteoprogenitor cells derived from stem cells were effective in supporting the integration of macroporous hydroxyapatite scaffolds in damaged bones. Three patients were treated using this method and CT scans taken 6 months afterwards showed good callus formation and integration of the interfaces in all patients [2].
Even more interesting were the results obtained by a team of scientists from the National Institutes of Health, Bethesda, USA, who managed to grow new bone from stem cells harvested from skin cells. The paper was published in the Cell Reports journal, the harvested skin cells being reprogramed into equivalents of embryonic stem cells [3]. The obtained iPSCs were treated in lab conditions to differentiate into precursors of bone cells, then transplanted the obtained cells into monkeys, on a ceramic scaffold.
The implanted cells grew new bone on top of the scaffolds, researchers finding no sign of tumor. According to the researchers, this technique has two great advantages: the stem cells harvested from patient’s own cells are less likely to be attacked by one’s immune system, and iPSCs can be generated from any individual.
Although the use of stem cells for speeding up the integration of implants in damaged bones is not new, scientists are now looking to develop these methods further, so as to obtain stem cells that can promote bone regeneration and regrowth once transplanted to humans.
References:
[1] http://gladstoneinstitutes.org/pressrelease/2015-05-11/scientists-regenerate-bone-tissue-using-only-proteins-secreted-by-stem-cells
[2] http://www.healio.com/orthopedics/biologics/news/print/orthopedics-today/%7B45aecb5d-a1c0-4e13-8bf7-607f32a812bf%7D/bone-regeneration-is-possible-using-stem-cells
[3] www.cell.com/cell-reports/abstract/S2211-1247%2814%2900306-4
- Published in Corporate News / Blog
A Good Night's Sleep Protects Stem Cells From Premature Aging
If you’re one of those people who is really fond of their beauty sleep, or who never compromises when it comes to getting their full eight hours per night, now you have one more reason to make a full night’s sleep a priority .
A study by scientists at the German Cancer Research Center have found that while environmental stress can damage the DNA in adult hematopoietic stem cells, a good night’s sleep can keep these cells young, contributing to a youthful appearance and preventing cancer.
Healthy sleep patterns lower the risk of DNA damage in stem cells
According to German researchers, under normal conditions a high number of different types of adult stem cells exists in a state of dormancy inside the human body, but they cannot divide, therefore cannot be used for tissue regeneration. This state of dormancy protects the stem cells from DNA damage, keeping us younger and preventing premature aging [1].
Yet, increased levels of stress in all its forms—from chronic infections to environmental stress—can trigger a rapid division of stem cells, kicked into gear as the body needs to repair its damaged tissues. In such conditions, the dormant stem cells go from no activity to very high activity in a short interval, and this rapid change forces them to increase their metabolic rate and synthesize new DNA.
Doctor Michael Milsom, who coordinated the German study, says that having to simultaneously execute such complicated functions increases the risk of DNA damage in the stem cells, reducing the ability of tissues to repair themselves and speeding up aging [1, 3].
Moreover, scientists believes that the accumulation of stress-induced damage in the stem cells can make one more prone to cancer. Experiments conducted in this study showed that cell division that takes place under stress leads to an increased production of reactive metabolites. These substances can damage DNA, causing the death of stem cells or leading to mutations that can contribute to cancer.
Understanding how to prevent the aging of stem cells or DNA mutations and damage could be the key to delaying the aging process and reducing the risk of developing certain forms of cancer, concludes Dr. Trumpp, co-author of the study’s research paper.
Protect your stem cells for healthy skin and a youthful appearance
The study is not the only one to prove a connection between sleep and the health of stem cells. Another paper, published in the journal of Cell Research by scientists from the University of California Irvine, showed that circadian rhythms regulate the metabolism of skin stem cells, and that getting enough sleep during the night can maintain healthy cell division, nurturing stem cell differentiation [2].
Although the study was conducted on mice, the findings are worth exploring further to determine whether a disruption in the healthy circadian rhythm can alter the normal function of stem cells, leading to accelerated aging.
Professors Andersen and Gratton, who conducted the Irvine study, focused on the effects stem cells have on the skin, already knowing that stem cells found in the dermal layers protect the skin and help in the repairing the epidermis after injuries.
Using innovative technologies, the two researchers measured the metabolic state of stem cells, discovering that the circadian clock does regulate one form of intermediary metabolism in target cells. According to researchers, it’s the same component of metabolism that creates oxygen radicals, harmful substances that can cause DNA damage.
The results of this study suggest that maintaining healthy sleep patterns can prevent DNA-damage in skin stem cells, while an altered internal clock could lead to the accumulation of damage in these cells, accelerating aging.
References:
[1] http://www.sciencedaily.com/releases/2015/02/150218122951.htm
[2] http://www.cell.com/cell-reports/abstract/S2211-1247%2814%2901018-3
[3] http://en.wikipedia.org/wiki/DNA_damage_theory_of_aging
- Published in Corporate News / Blog
Using Bone Marrow Stem Cells to Treat Heart Disease
What seemed an impossible medical challenge a few years ago might turn into a do-able task with the help of bone marrow stem cells. Several trials are testing the use of adult stem cells in heart disease, hoping to identify a viable solution for repairing the cardiac tissue damaged by heart attacks, coronary artery disease and other similar ailments.
<h1>Obtaining cardiac muscle cells in the lab</h1>
Despite the huge amount of information available out there and the numerous health programs that aim to prevent heart diseases, these conditions remain the most common cause of death in Europe, with heart attacks dominating the list. According to statistics, around 7 million people worldwide suffer from heart attacks each year, the damage being in lots of cases irreversible.
Given the amazing results obtained with stem cell therapies in conditions like leukemia or lymphoma, it was natural for scientists to intensify their research efforts in this niche, in order to see whether the potent stem cells can also be used for repairing damaged hearts. While some studies have showed promising results, others have found no improvement after transplanting stem cells to patients with heart conditions.
The biggest challenge in these cases seems to be the reprograming of stem cells obtained from other tissues into cardiomyocytes. Cardiomyocites are the cells that form the cardiac muscle, and although for a very long time scientists believed that the heart does not produce any stem cells, it’s been shown that the body does produce new cardiomyocytes each year, but the number decreases with age.
The discovery that the human heart produces new cells each year has created hope and encouraged researchers to try to find out where the new cardiac cells come from and how this process is controlled inside the body. The ultimate goal was to identify those mechanisms that could be replicated in lab conditions, so as to obtain new heart cells viable for transplantation in patients with heart diseases.
Although the existence of heart stem cells has not been confirmed yet, it is possible to obtain cardiomyocytes in the lab, from stem cells obtained either from embryos or from iPS cells (induced pluripotent stem cells). The latter can be obtained by reprogramming skin cells that are taken directly from the patient, reducing the risk of transplant rejection.
One of the biggest problems here comes from the fact that bone marrow cells and other adult stem cells can be reprogramed to repair a specific tissue, but if they are treated in lab conditions until they differentiate to specific cells like those in the cardiac tissue, the risk of tumors and rejection increases.
On the other hand, if the pluripotent stem cells from embryos or the iPS cells are transplanted into the heart, they might differentiate and give birth to a multitude of cells. It is impossible for one to control the type of cells formed by stem cells in the body once transplanted, if those cells were transplanted before specializing.
Stem cell studies on the damaged heart show mixed results
Existing studies show that treating heart conditions with stem cells is more difficult than using stem cells therapies for other tissues and organs. A trial done in Belgium, Switzerland and Serbia on 45 patients aimed to treat heart attack victims with stem cells. The injected cells led to no complications and were guided to become cardiac cells, scientists highlighting the safety and feasibility of the procedure [1].
Other studies showed little to no effect after the transplantation of stem cells. Cardiologist Darrel Francis at Imperial College London published a review study in BMJ, examining 133 reports of 49 randomized clinical trials that aimed to treat heart attack or heart failure patients with stem cells. According to his paper, more than 600 discrepancies were found in these trials, so the results cannot be considered relevant [2].
Francis’ study showed that the 5 trials that had no discrepancies reported no improvement in the left ventricular ejection fraction (LVEF) after stem cell treatment, while the 5 trials with the most numerous discrepancies reported a significant improvement (+7.7%) of LVEF after stem cell therapy.
While scientists are still trying to answer whether stem cells are a solution for damaged heart tissue, some stories report that patients who received this treatment after a heart attack saw a clear and dramatic improvement in their health state and heart function. One of these patients is Jim Dearing of Louisville, who was among the first patients to receive heart stem cells after suffering two heart attacks and heart failure. His heart was functioning normally one year post treatment [3].
What’s certain for now is that results of these studies are mixed, and researchers will need to further investigate the use of stem cells from bone marrow in patients with heart diseases.
References:
[1] https://beyondthedish.wordpress.com/2014/12/03/mayo-clinic-uses-reprogrammed-stem-cells-to-heal-the-heart/
[2] http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4002982/
[3] http://www.webmd.com/heart/features/stem-cells-heart-failure-heart-disease
- Published in Corporate News / Blog
The different types of stem cells and their current uses
 Stem cells offer great potential for use in clinical applications thanks to their ability to specialize into different cell types and to renew themselves. Although some of them have limitations, stem cells are still an amazing resource for the medical world, as no other cell inside the human body has the ability to generate new cell types with a more specific function that the source.
Stem cells offer great potential for use in clinical applications thanks to their ability to specialize into different cell types and to renew themselves. Although some of them have limitations, stem cells are still an amazing resource for the medical world, as no other cell inside the human body has the ability to generate new cell types with a more specific function that the source.
Stem cells can be considered the body’s raw building blocks, as all the other cells with specialized functions result from stem cells that divide and give birth to daughter cells. These cells, at their turn, divide or differentiate and become specialized, giving birth to muscle, bone, blood, brain or other specific cell types.
The characteristics and applications of stem cells vary not only depending on the type of cells they differentiate into, but also on the nature of the tissue they are derived from. From this point of view, stem cells can be classified into three main groups: embryonic, adult and induced pluripotent stem cells.
Types of stem cells depending on origin
Embryonic stem cells (ESCs) come from embryos of up to 5 days old, and are pluripotent, meaning that they can divide into several stem cells and specialize into any type of cell. This property allows embryonic stem cells to repair damaged tissues and organs and to stimulate the regeneration of diseased tissues. Researchers can grow and induce the differentiation of ESCs in the lab, but the use of embryonic stem cells is often avoided due to ethical considerations.
Adult stem cells, the second type, are found in adult tissues inside the human body and they can also differentiate into various cell types, but their ability to give birth to new cells is limited. Although until recently it’s been thought that an adult stem cells can only differentiate into the same type of cell as the tissue it comes from, emerging studies suggest that these cells, just like ESCs, can create unrelated cell types.
In other words, just like an embryonic stem cell derived from bone marrow can give birth to liver or muscle cells, adult stem cells taken from bone marrow can create bone or skin cells. There’s a limit though, as adult stem cells can’t be manipulated as efficiently as ESCs, and they’re not as versatile and the ones derived from embryos.
The third type of stem cells is somewhere in between the adult and embryonic stem cells, and it’s called induced pluripotent stem cells (iPSCs). These are highly versatile, similarly to ESCs, but are made from adult specialized cells through laboratory techniques (genetic reprogramming). iPSCs have two main advantages: first one’s that they do not create any ethical debate, as they don’t come from embryos, and the second one is that the risk of rejection is lower than in adult stem cells, thanks to the fact that iPSCs are reprogrammed to act as ESCs.
Current applications of stem cells by type
We won’t discuss the ESCs here as the tendency is to not use embryonic stem cells, and opt for adult or induced pluripotent stem cells instead.
Perhaps the most used of all adult stem cells are those obtained from the bone marrow (mesenchymal stem cells), which can be differentiated into bone, cartilage and fat cells, and can encourage the production of new blood cells. These were not proven to be able to differentiate in any type of cell inside the human body, but existing research suggests mesenchymal stem cells may be useful in bone and cartilage repair or blood vessel repair after a heart attack [5].
In lab studies, bone marrow stem cells from adult rats were able to partially regrow the damaged liver, and to have beneficial effects when injected into the damaged heart. Also, scientists at the Children’s Hospital Boston have found adult bone marrow stem cells to protect against chronic lung disease [2] in mice models.
Induced pluripotent stem cells have also been tested for their ability to differentiate, and lab results showed that iPSCs made from skin samples may be useful in treating neurological disorders like Parkinson’s disease or Down’s syndrome [8].
Researchers in Japan managed to generate human liver buds from induced pluripotent stem cells, the scientists using three different types of stem cells for this purpose: part of them were hepatocytes coaxed from iPSCs, others were endothelial stem cells and others were mesenchymal stem cells. The liver buds were grown in vitro for a few days then transplanted to mice, where they quickly connected with the blood vessels and continued to grow.
Other studies have shown that iPSCs grown from embryonic cord-blood cells can be used for repairing the damaged retina of mice and regrowing the vascular vessels. Scientists from the Japan Ministry Health are currently conducting a clinical trial using autologous iPSCs in six patients affected by age-related macular degeneration. IPSCs used for this trial are derived from skin cells, and reprogrammed to differentiate into retinal pigment epithelial cells.
Adult stem cells have been used in treating leukemia and blood or bone related cancers utilizing bone marrow transplants [1]; mesenchymal stem cells have been shown to help in repairing the damaged cartilage in patients with articular cartilage defects [3] and to improve the outcome in spinal cord injuries [4]. Peripheral vascular disease [6] and liver cirrhosis [7] may also be treatable with adult stem cells.
Although adult stem cells and iPSCs can be differentiated in a wider variety of cells, not all of them have been tested in human subjects, one of the biggest barriers being the potential immunological rejection.
References
[1] http://en.wikipedia.org/wiki/Adult_stem_cell
[2] http://www.childrenshospital.org/news-and-events/2009/december-2009/bone-marrow-stem-cells-may-prevent-chronic-lung-disease
[3] http://www.ncbi.nlm.nih.gov/pubmed/18038395
[4] http://www.pubstemcell.com/monthly/006030700113.htm
[5] http://stemcells.nih.gov/info/scireport/pages/chapter9.aspx
[6] http://www.ncbi.nlm.nih.gov/pubmed/21671823
[7] http://www.ncbi.nlm.nih.gov/pubmed/16778155
[8] http://www.eurostemcell.org/factsheet/stem-cell-research-therapy-types-stem-cells-and-their-current-uses#iPS
- Published in Corporate News / Blog